-
Golfer Suddenly Withdraws During 2nd Round of Valspar Championship - 20 mins ago
-
What BTS Is Wearing for Its Comeback Concert and Why - 38 mins ago
-
California water regulators reexamine why Mono Lake hasn’t rebounded - 42 mins ago
-
Nancy Guthrie Update: FBI ‘Ask Questions About Vacant Property’ - 55 mins ago
-
Americans Deserve the Truth About Iran - about 1 hour ago
-
Music teacher, 93, “still approaches the world with the curiosity of a child.” - about 1 hour ago
-
Covering murals, removing statues: The erasure of Cesar Chavez is underway in California - 2 hours ago
-
How Camping Trip Left Utah Mom of 3 With $50K Bill and CDC Warning - 2 hours ago
-
Spring Awakening – The New York Times - 2 hours ago
-
David Botstein, Gene-Mapping Pioneer, Dies at 83 - 3 hours ago
How Camping Trip Left Utah Mom of 3 With $50K Bill and CDC Warning
A camping trip in Northern Arizona took an alarming turn for one family, leaving them with a CDC warning an a hefty $50,000 bill as a result.
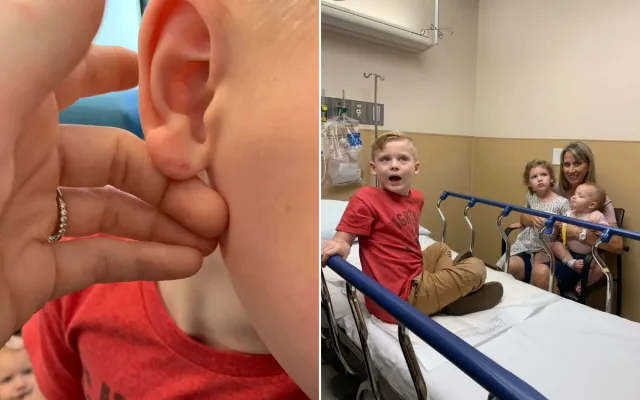
Katy Monson, a mom of three and clinical laboratory scientist from Utah, got up one morning back in 2019 to a disturbing sight. “My 5-year-old woke up with two mysterious red dots on his earlobe,” Monson told Newsweek.
The two piercing marks looked like they had been made by a bat. The family had been on a camping trip in Arizona and, as Monson recalled, there had been issues with bats getting into their cabin. At one point, they had found what they now suspect to be bat droppings outside their room.
That was more than enough to spark Monson into action. “I drove our son to our pediatrician,” Monson said. “He measured the distance. and it matched an Arizona brown bat bite width.”
That was when the phone calls began. Monson found herself “inundated” with calls from the CDC [Centers for Disease Control and Prevention] and Utah State Department of Health encouraging not only her son but the entire family to get rabies shots.
“A farmer had died in 2019 from a bat licking his thumb near an abrasion, and he succumbed to rabies in a local hospital, leading to the state taking this all very seriously,” Monson said. “They sternly encouraged us all to get post-exposure vaccinations since not all exposures leave a mark.”
While rabies is well controlled in the U.S., the CDC estimates that more than 4 million Americans report being bitten by animals each year. Though rabies in humans is completely preventable, it is essential that anyone even suspecting they may have contracted it gets medical help right away. The treatment is called post-exposure prophylaxis (PEP), and it is highly effective if administered as soon as possible after exposure.
Monson and her family were instructed to head immediately to Intermountain Medical Center (IMC) in Utah for emergency treatment. Unfortunately, as Monson would discover, for a family of five, it is expensive, even with insurance. When the mom first contacted United Healthcare, her family’s health care provider, while at IMC to check the treatment would be covered under their plan, she said: “They assured us it would be covered, but still had no access to our specific plan.”
In the meantime, her family was administered immunoglobulin and anti-rabies vaccines, as time was of the essence. At that point, however, Monson was still unable to give specific health plan information to the hospital to check coverage or send to the billing department.
Monson said she spent the best part of a day on the phone with her family’s health insurance provider to “try and ensure the cost was as low as possible and coded as ‘in network.’”
“I called five different facilities in the state to get bids for the shots, eventually having to get the shots from a children’s hospital in Salt Lake City, since our three children couldn’t receive the vaccine from the state facility,” Monson said.
Over the next 14 days, her kids had a series of shots, with each adding to the final billing amount for the family’s treatment. Monson said she applied for financial aid from Intermountain and the University of Utah but was denied by both.
By then, the total, unadjusted costs of the procedures had reached $50,109.24. That not only exceeded their family deductible of $2,700—the total amount a family must pay for covered health services in a plan year before the insurance company begins to pay costs—but also reach our “out of pocket maximum” of $13,300—the highest amount you pay for covered health services in a plan year, including deductibles, copayments, and coinsurance.
Monson contacted Intermountain who said “the best” it could do was offer a 10 percent discount. By then, Monson had already been crunching the numbers on the bill they had received, researching what was the “fair market price of each procedure.”
“Intermountain charged anywhere from double to quadruple the fair price,” Monson said. She added that, when she put that to an Intermountain representative on the phone, “she said that our insurance would have denied covering them if that were the truth and that, since they have already adjusted and agreed, she couldn’t do anything else.”
Newsweek has contacted Intermountain for comment.

Monson spent countless hours over the next few months on the phone to United Healthcare, Intermountain and the University of Utah Healthcare to try to bring the costs down as much as possible and ensure the family had been covered as much as possible by her health insurance.
Ultimately, despite her best efforts, Monson and her family were left saddled with a $13,300 bill that took two years to pay off. Seven years on, the mom still feels conflicted about the experience.
“We are all healthy and grateful to be past the whole ordeal,” she said. “The devastating part was how much I prepared and negotiated before receiving the bills, and how little power I had once I received them.”
As someone who has worked in hospital labs all of her career, Monson has seen the “altruistic” side of health care. Having experienced first hand the exorbitant prices attached to medical care and the way insurance companies can deny cover to those paying thousands in premiums, she has now also seen the other side of it all, and it’s not pretty.
“As patients, we have little power with so many pockets being filled in our time of need,” Monson concluded.
Source link